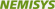Children and their families all have a unique story to tell made up of
their own particular circumstances and experiences and their responses
to these. These stories need to be told and the ICPCN wishes to build
up a collection of such narratives from around the world. The hospice
environment, services offered and access to resources may alter from country to country, but
children are children wherever they are and the love, the anguish, the
hope, the moments of joy and the depths of sorrow that a parent feels
when a child is diagnosed with a life-limiting illness is a universal
language.
Our wish is that these stories about real children and the hospices who care for them will not only put a
"human face" to the work that is done by children's palliative care
services worldwide, but may also allay fears and bring some comfort and hope to families
out there who feel they are alone.
We are most grateful to the parents and other loved ones who have so bravely shared their stories with us. Should you wish to add your story to this collection, please do not hesitate to contact our Information Officer at info@icpcn.co.za
Sam's Story (UK)
Ayanda's Story (South Africa)
Initially there was hope that the treatment would work but soon after Ayanda’s 3rd birthday the cancer reoccurred and he was readmitted to hospital where they found the cancer had spread to other parts of his body. Ayanda’s parents were given the sad news that there was little more that could be done and Ayanda was discharged from the hospital. No explanation was given of what might happen next and what to do in order to help their son in the last weeks or months of his life. Bewildered, they left the hospital with a bottle of paracetamol and a very sick child.
Dr Julia Ambler, a paediatric palliative care specialist with Bigshoes describes finding Ayanda “very symptomatic and in lots of pain that was uncontrolled.” She goes on to explain that they were able to get his pain under control and when he was feeling better they could start discussing what the family wanted for him. “They were aware that he was going to die at some stage.”But for us it is about where they wanted to have that care in those last days and about Ayanda’s quality of life,” she says.
For the first time since his diagnosis, Ayanda’s parents were involved in the decision making around his care and treatment. They chose to have Ayanda die at home rather than in the hospital and were empowered to give him his pain medication. They were helped to draw up a full plan of what to do in an emergency and in any unexpected eventuality.
Dr Ambler sums up by saying: “So how palliative care made a difference ... is that they firstly got to understand what was going on. Then they got to be involved in the decision making and at the end of the day they had a child that was really comfortable and who died at their own home, which was their choice."
* Names have been changed
Watch a YouTube video of Dr Julia Ambler telling Ayanda's story.
Alec's Story (Australia)
 Theresa McEwan, Alec McEwan and Lizzie Swatland
Theresa McEwan, Alec McEwan and Lizzie Swatland
Hi my name is Theresa McEwan and I live on the Gold Coast of Australia. We have a local charity called Paradise Kids who support children and families experiencing grief or loss. In 2005 my 7 year old son Alec was diagnosed with an aggressive form of Multiple Sclerosis and went into Pallative care. My beautiful son went from a healthy 7 year to a very disabled child. During this time I gave up work to care for my son full time as his health continued to deteriorate. I am so grateful for this time with Alec. “We lived a life-time in a day” We lived a life-time in a day and captured many memories together. As a Mum facing the thought of losing my beautiful boy it was with gratitude that Paradise Kids was recommended to my family.
I was introduced to Lizzie Swatland who wrote a program called: “lllness Support Program”.The program caters for children with a life limiting or terminal illness. Volunteers implement this program in either the hospital or at home over 7 sessions. The program takes an holistic approach with an emphasis on children understanding that they are more than their physical symptoms.
Since my son’s passing I have been very fortunate to volunteer with Paradise Kids and offer support to other families in a similar situation. I have found this very rewarding and it has also helped me in my journey through healing.
Losing a child is beyond comprehension but it is Alec’s memory that enables me to help others. Recently I have started working at Paradise Kids 3 days a week and it is a privilege to be able to contribute my experiences to help others. Paradise Kids conducts grief and loss courses throughout the year catering to children of all ages. We have a hospice that accommodates 8 adults on the premises. We are committed to educating the community and implement several courses including a Palliative Care Training Program. We are currently completing a new holiday house to accommodate children with a terminal illness and their families. During their stay the families will be offered support through counselling and the programs that Paradise Kids have to offer.Paradise Kids is a local charity that relies on donations from the public to continue their vital work in the community.
Visit the website at : http://www.paradisekids.org.au
Andrea's Story (Norway)
 Andrea and her mother, Natasha PedersenWe live in a technological world where medical equipment will only get better and more advanced. Luckily, most people do not get to know anything about this as they do not have a child with an incurable illness. However, although the number of deaths have drastically reduced, every year there are 600 children who die in Norway from a serious illness. Nobody can be fully prepared for death, and especially not that of one’s own child. Following many of my own experiences as a parent, a previous health-worker and a priest, I have observed that there is a lack of assistance for that group of children and their families. The purpose of the organisation, Yes to Pallliative Care and Units for Children in Norway is first and foremost to bring our case and our needs to the fore.
Andrea and her mother, Natasha PedersenWe live in a technological world where medical equipment will only get better and more advanced. Luckily, most people do not get to know anything about this as they do not have a child with an incurable illness. However, although the number of deaths have drastically reduced, every year there are 600 children who die in Norway from a serious illness. Nobody can be fully prepared for death, and especially not that of one’s own child. Following many of my own experiences as a parent, a previous health-worker and a priest, I have observed that there is a lack of assistance for that group of children and their families. The purpose of the organisation, Yes to Pallliative Care and Units for Children in Norway is first and foremost to bring our case and our needs to the fore.
We do not know what tomorrow brings, and being fortunate to have been a mother for 17 years to a child with multiple handicaps who has lived with one foot in the grave, I have experienced this fact with both mind, body and soul. I have experienced unnecessary suffering and stress simply due to a lack of knowledge. To provide a worthy and dignified end for a child’s life is very difficult as the fear of the unknown is always there! A child’s death will always be difficult, but without knowledge and support, it becomes far more difficult than it needs to be.
When one waits for death, sorrow is great and one suffers anticipatory grief. I may have the knowledge about death as a priest and a care-giver, but this has not helped me a great deal in the daily life of my family. One is first and foremost a mother, a relative, and a human being. It is hard when, after years of treatment and focusing on correcting and preventing conditions, suddenly you have to put all your energy into focusing just on the child and not so much on her treatment. It confronts us as adults, as parents and has health workers. That a child shall die is against nature, and it involves many strong feelings in us.
Andrea, who is my mentor and daughter, has now lived a long life with uncertainty hanging over her. In the spring of 2008, the decision was made not to put Andrea on life-support. Even though we have lived so long with a sick child, this was a very difficult process for us to go through, involving many meetings and much heart searching. Three doctors at the hospital and Andrea’s primary doctor prepared, together with ourselves, a plan to allow the rest of her life to be as easy as possible. The plan gave us reassurance about when things should happen, and the changes that would occur. Now, here we are, one year later, and Andrea is still with us with seven different diagnoses, two of which are fatal. The State Hospital told us this autumn 2009 that her life and her health are untreatable and getting worse. This touches us deeply and now we have arrived at the most difficult stage in Andrea’s life. We know that she is about to die, she has been close many times, and all the medical alarms are showing red. We feel so helpless and know that all we can do now is to fight to ensure that she receives a worthy and dignified end to her life.
MOTIVATION TO START THE ORGANISATIONWhile a great deal is known about adult palliative care, particularly for those suffering from cancer, there is not enough knowledge about how children who have untreatable illnesses feel in Norway. And the differences and variations in the diagnoses of these children are huge. Many children are unable to talk; some are blind or deaf and have enormous challenges communicating. These children require extra help from those around them, health workers, family, doctors and other professionals. They need help to see, listen and touch, and for someone to just BE there. We, who have worked with language, know that non-verbal language is amazingly strong.
ANDREA’S LEGACYAndrea now holds the last baton, and we are fighting to get a bureaucratic system to help us establish an organisation so that children who are dying are able to receive good quality palliative care from trained health care workers. The idea for such a group grew in me throughout this process over many years and many sleepless nights! To lose that which is the dearest to you, your own child, is heartbreaking. We have begun this group for our own benefit as well as for all the others who suffer as we do. It is most unlikely that we will get the help and support we need for our own child, but we know that it is still important for those who will come later. This will be Andrea’s legacy to the children in Norway.
Natasha Pedersen Just a mother and founder of Yes to Palliative Care and Units for Children in Norway
February 2010
Andrea, the child responsible for the founding of “Yes to Palliative Care and Units in Norway”, died in her mother and father’s bed, February 7th 2010, aged 17 years. Natasha and Jim, her parents will continue to work for palliative care for all the children of Norway. The funeral was beautiful, the church was packed full of friends and family and others who wanted to pay their last respects. Her very best friend, Winnie the Pooh (Andrea was his biggest fan) was the guard of honour and followed her to Heaven.
The very same day that Andrea was buried, our government finally talked about a “Plan to Help Living”, which will occur on 2 March 2010. Several times our organization has been mentioned in the Norwegian Parliament. In a very short time, we have accomplished a lot! We are working on translating books and literature, which we will sell to doctors and health workers as soon as possible. One of our goals is to raise enough money so that we can travel around the country and teach doctors, parents, sisters and brothers how to give the best possible care to the sick child. And last, but not least, start a support-group for everybody who is, and will be, in this situation.
Our work will continue in Andrea`s spirit.
Froeydis Vatne GrahamMember of the Board “Yes to Palliative Care and Units in Norway”
Theara's Story (Cambodia)
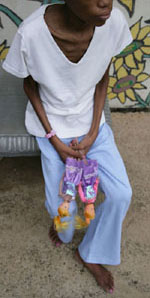
 Theara Sok with her grandmotherWhile in Cambodia volunteering for Cambodian Children's Fund (CCF), I became involved in a tragic situation around a 14 month old baby girl named Theara Sok. She was from Kompong Cham province and had been diagnosed with a kidney tumor at a free children’s hospital in Phnom Penh.
Theara Sok with her grandmotherWhile in Cambodia volunteering for Cambodian Children's Fund (CCF), I became involved in a tragic situation around a 14 month old baby girl named Theara Sok. She was from Kompong Cham province and had been diagnosed with a kidney tumor at a free children’s hospital in Phnom Penh.
Upon diagnosis, Theara was referred to another hospital in Phnom Penh which was the only hospital in Cambodia that treats cancer. Her mother took her to this hospital which confirmed Wilms cancer but would not treat her because of her young age. They do not treat any child under the age of 3 years - a fact which I have since verified via several other sources.
After being turned away by the hospital, we took Theara to a private clinic to get a further medical opinion and we were asked to provide CT scans from yet another hospital to better evaluate her condition. These scans sadly confirmed that her cancer was advanced and nothing that could be done for her in Cambodia. We were told that although there would have been treatment options available in the West, in Cambodia, there was nothing more that could be done. A friend at CCF who has personally endured the losses of babies from various causes, told me; “Rick, no matter how determined you are, there comes a time when you have to accept that there is nothing more you can do.” As painful as the decision was, I knew he was right. We took her home to her province to prepare for her inevitable passing, one of the most emotional experiences of my life. On our arrival, we were greeted by her entire family on the road and invited into their small wooden home. As we all sat around her on the floor, my Cambodian friend explained the sad news to the family. The adults were tearful but held their composure for the sake of the children in the room.
After the head of the family expressed gratitude for what we had done to help Theara, he took my hand and put it on hers. She grabbed my finger with her tiny hand and as we sat there around her on the floor holding back the tears, the “oneness” that I felt with this family I had just met was unlike anything I have felt before. We all seemed to be connected by the love for this little girl on a level that was not of this world.
With no experience in the medical profession, via email I enlisted the help of a friend and volunteer who is a pediatric oncologist in America. I asked her to provide me with assistance for pain management to make Theara as comfortable as possible as this vicious disease attacked her tiny body. She gave me a list of several pain medications and dosages, including morphine for the final stages to help ease her suffering. I also enlisted the help of a certified nurse who would be able to properly administer these medications.
In attempting to begin pain management, we were stunned and frustrated to learn that the only medication we could obtain was simple codeine syrup. We tried various pharmacies and even went back to the hospitals we first took Theara to, and were told that these items were not available in Cambodia….not even morphine.
For the next 4-5 weeks, I made regular trips to Theara’s family’s home in Kompong Cham to bring her the codeine syrup and other needs such as baby formula. With every trip, her condition worsened. On what turned out to be my last trip to her home to provide medication, she was a mere skeleton of the beautiful little girl I first met only several weeks earlier. She was having an extremely hard time breathing. I received a phone call about 3 days later from her family informing me of her death. While expected, it was still one of the most painful phone calls I ever received. Through my tears, the only comfort I found was that she was not longer suffering.
After Theara passed on, I vowed to do something in her name so that other Cambodian babies stricken with cancer or other terminal diseases do not die the same horrible and painful death as she did. Although sad, I am at peace in knowing that we did not walk away from Theara in her time of need and we exhausted all options. Still, I am haunted by the fact that we could not do more, especially in comforting her when her passing was imminent.
Theara’s legacy
I do not know why, of all people, she was brought to me, but I will remember this little angel always as she has forever changed my life. I am a firm believer that everything that happens in a person’s life is for a reason and I am determined to do all I can to ensure that as many Cambodian children as possible never have to suffer as Theara did. Although I would ultimately like to see a pediatric cancer treatment facility in Cambodia, I have realised that the greatest need right now is the establishment of a hospice program. After further research I have discovered that Theara’s suffering is commonplace in sick babies, especially the poor.
My hope is that this hospice can eventually assist in giving the end-of-life quality and dignity that every person deserves.
Theara's Story was written by Rick Peterson who plans to open a hospice in Cambodia called "Theara's Light" in Theara's memory.
You can contact Rick at: Richard_Pete011@msn.com
 Andrea and her mother, Natasha Pedersen
Andrea and her mother, Natasha PedersenFebruary 2010
Andrea, the child responsible for the founding of “Yes to Palliative Care and Units in Norway”, died in her mother and father’s bed, February 7th 2010, aged 17 years. Natasha and Jim, her parents will continue to work for palliative care for all the children of Norway. The funeral was beautiful, the church was packed full of friends and family and others who wanted to pay their last respects. Her very best friend, Winnie the Pooh (Andrea was his biggest fan) was the guard of honour and followed her to Heaven.
The very same day that Andrea was buried, our government finally talked about a “Plan to Help Living”, which will occur on 2 March 2010. Several times our organization has been mentioned in the Norwegian Parliament. In a very short time, we have accomplished a lot! We are working on translating books and literature, which we will sell to doctors and health workers as soon as possible. One of our goals is to raise enough money so that we can travel around the country and teach doctors, parents, sisters and brothers how to give the best possible care to the sick child. And last, but not least, start a support-group for everybody who is, and will be, in this situation.
 Theara Sok with her grandmother
Theara Sok with her grandmotherFelix's Story (Germany)
 Felix and his parentsThis year I met a young couple struggling bravely with their fate. They are a happy family, who love their son dearly but who were feeling completely exhausted and isolated and who were struggling to make ends meet on their income as a result of having to pay for the necessary medicines for their son. Their two-year-old son, Felix, was born with a severe brain defect and has a life expectancy of only a few months. The parents are both in their early twenties and trying their best to manage on their own. They explained to me just how desperate they feel. The mother is alone with their child all day long and they cannot sleep through the night because of the care-needs of their disabled son. They also told me that they have enormous problems getting the correct medicine for their child. It is far too expensive to buy it legally, and so they attempted to import it from a cheaper source. Now, the young father has to deal with being accused of importing illegal drugs. Their story is symbolic of the situation faced by many such families. Families in similar situations become more and more socially isolated and lack the courage to get in touch with possible support systems.
Felix and his parentsThis year I met a young couple struggling bravely with their fate. They are a happy family, who love their son dearly but who were feeling completely exhausted and isolated and who were struggling to make ends meet on their income as a result of having to pay for the necessary medicines for their son. Their two-year-old son, Felix, was born with a severe brain defect and has a life expectancy of only a few months. The parents are both in their early twenties and trying their best to manage on their own. They explained to me just how desperate they feel. The mother is alone with their child all day long and they cannot sleep through the night because of the care-needs of their disabled son. They also told me that they have enormous problems getting the correct medicine for their child. It is far too expensive to buy it legally, and so they attempted to import it from a cheaper source. Now, the young father has to deal with being accused of importing illegal drugs. Their story is symbolic of the situation faced by many such families. Families in similar situations become more and more socially isolated and lack the courage to get in touch with possible support systems.
Their story is just one of many, which is why I want to plead for children’s hospices and children’s hospice organisations to become more visible. Children's hospice and palliative care services need to let people know what is available to them and to offer counselling to people.
 Felix and his parents
Felix and his parentsWritten by Sabine Kraft, Executive Director of Bundesverband Kinderhospiz in Germany
Bayu's Story (Indonesia)
A story from Indonesia of a brave young girl who was the very first patient at Rachel House's inpatient facility.
Bayu (2001-2009)
- Whether transfusions would alleviate the symptoms of discomfort for Bayu?
- And, questions should be posed on the purpose of the blood tests before they were ordered
Adi's Story (Indonesia)
The story of a girl whose name meant "Unwanted" in South Sotho (South Africa)